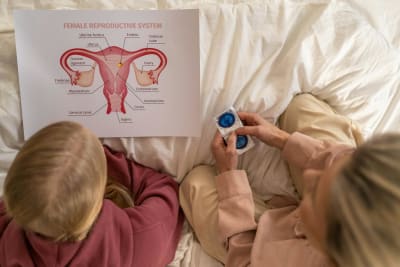
For decades, whispers of irregular cycles, persistent acne, and unexplained weight fluctuations have been a shared, often frustrating, experience for countless women. These symptoms, dismissed by some as mere inconveniences, are frequently the early indicators of Polycystic Ovary Syndrome (PCOS), a complex hormonal disorder that impacts reproductive health, metabolism, and overall well-being. While the condition has been recognized in medical circles for years, its nuanced presentation and profound systemic implications are only now being fully appreciated, moving beyond a simple gynecological issue to a broader public health concern. PCOS is far from a new phenomenon, with its roots tracing back to early 20th-century medical observations. Initially characterized by a triad of symptoms – irregular periods, ovarian cysts, and excess male hormones – the understanding of PCOS has evolved significantly. It's now understood as a spectrum disorder, often involving a delicate imbalance in reproductive hormones, particularly androgens, which can disrupt the normal menstrual cycle and ovulation. This hormonal dysregulation is intrinsically linked to metabolic issues, affecting how the body processes insulin and leading to increased insulin resistance, a critical factor in many of the syndrome's manifestations. Data consistently points to the widespread nature of PCOS. The Office on Women’s Health estimates that PCOS affects approximately 1 in 10 women of childbearing age, making it one of the most common endocrine disorders in this demographic. This staggering figure underscores the urgency of comprehensive research and accessible healthcare. Beyond reproductive challenges, which can include infertility or difficulty conceiving, the long-term health risks associated with PCOS are substantial. These include a significantly elevated risk of developing type 2 diabetes, heart disease, sleep apnea, and endometrial cancer, highlighting the systemic reach of this hormonal imbalance. The diagnostic journey for PCOS can be lengthy and disheartening for many. Because its symptoms are varied and can overlap with other conditions, women often face years of uncertainty and misdiagnosis. A typical diagnostic pathway involves a thorough review of menstrual history, physical examination for signs of excess androgens like acne and hirsutism (excess hair growth), blood tests to measure hormone levels, and sometimes an ultrasound to examine the ovaries. However, the diagnostic criteria themselves have been debated, with different medical bodies sometimes employing slightly varied guidelines, which can lead to further confusion and delayed diagnosis for some individuals. Stakeholder perspectives reveal a growing call for more integrated care models. Dr. Anya Sharma, an endocrinologist specializing in reproductive health, notes, "We're moving past a purely gynecological lens. PCOS affects virtually every system in the body, from the brain to the gut. A multidisciplinary approach involving endocrinologists, dietitians, mental health professionals, and primary care physicians is essential for effective management." Patients themselves often bear the brunt of systemic neglect. Sarah Chen, a 32-year-old diagnosed with PCOS five years ago, shared her experience: "I struggled for nearly a decade with debilitating fatigue, painful acne, and weight that just wouldn't budge. Doctors initially dismissed it as stress or diet. It wasn't until I saw a specialist who understood the hormonal connection that I finally got a diagnosis and felt seen." The deeper systemic issue revealed by PCOS is the historical underfunding and fragmented approach to women's health research and care. For too long, conditions primarily affecting women have been siloed within specific specialties or relegated to secondary research priorities. This has resulted in a knowledge gap and a lack of coordinated care pathways, leaving millions to navigate complex health challenges with insufficient support and understanding. Looking ahead, the focus is shifting towards earlier detection, personalized treatment strategies, and a greater emphasis on lifestyle interventions. Research into the genetic and environmental factors contributing to PCOS is ongoing, aiming to identify predispositions and develop preventative measures. Furthermore, greater public awareness campaigns are crucial to destigmatize the condition and empower women to advocate for their health, ensuring that the diverse and profound impact of PCOS is recognized and addressed comprehensively within the healthcare landscape.
In Brief
Explore the complex hormonal disorder PCOS, its widespread impact on women's health, and the systemic challenges in diagnosis and care.Advertisement





Comments
No comments yet. Be the first to comment!